The European Health Data Space and the Primary Use of Health Data – From regulatory vision to clinical reality
Introduction
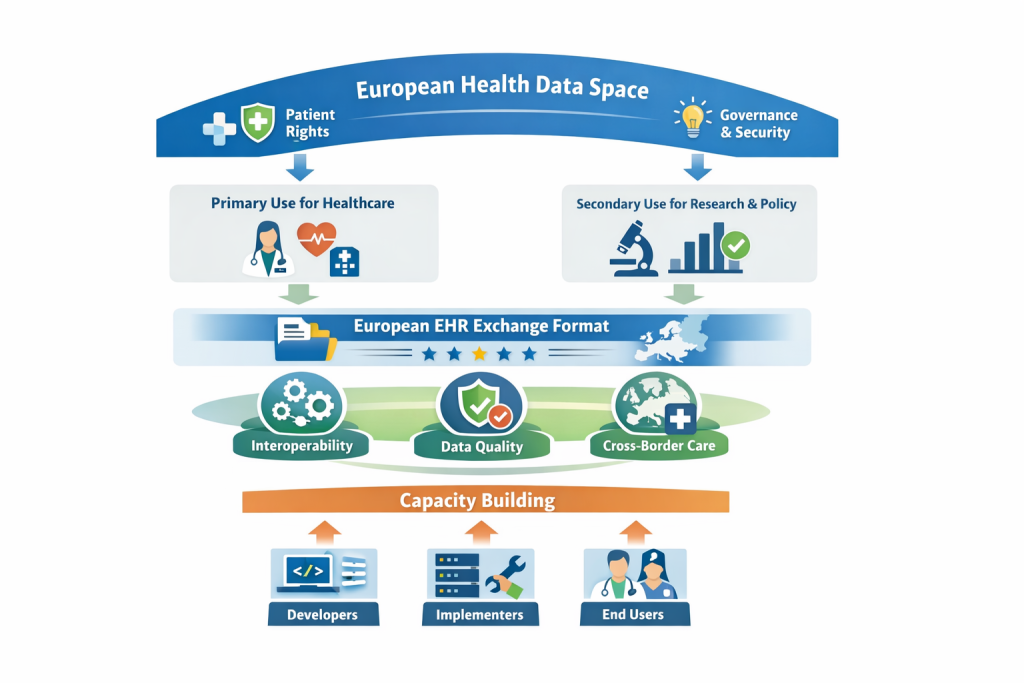
The European Health Data Space (EHDS) is one of the most ambitious digital health initiatives ever undertaken by the European Union. Adopted in 2025, the EHDS establishes a common legal, technical, and governance framework for the use and reuse of electronic health data across Europe. Its objectives are twofold: to strengthen the primary use of health data for care delivery and to enable the secondary use of health data for research, innovation, and policymaking.
While much attention has been paid to secondary use, the success of the EHDS will depend first and foremost on its impact on primary use—that is, the use of health data to provide healthcare services directly to individuals. This article focuses on how the EHDS reshapes primary use, what it requires from health systems and professionals, and why skills and interoperability readiness are critical to its implementation.

What is the European Health Data Space?
The EHDS is a Regulation of the European Union that creates a harmonised framework for accessing, exchanging, and using electronic health data across Member States. Unlike previous initiatives that relied mainly on voluntary coordination, the EHDS introduces binding obligations for national authorities, healthcare providers, and digital health system vendors.
At its core, the EHDS seeks to ensure that individuals can access and share their health data seamlessly across borders, while healthcare professionals can rely on interoperable, trustworthy, and secure digital infrastructures. To achieve this, the Regulation establishes:
- A common set of individual rights over electronic health data
- Mandatory interoperability and security requirements for electronic health record (EHR) systems
- A governance structure at EU and national level
- A clear distinction between primary use and secondary use of health data
Primary use is the foundation upon which all other EHDS ambitions rest.
Defining primary use under the EHDS
Primary use refers to the processing of electronic health data for the provision of healthcare. This includes diagnosis, treatment, care coordination, and continuity of care within and across Member States. Under the EHDS, primary use is no longer confined to national systems or bilateral agreements; it becomes a European-wide capability.
The Regulation strengthens and expands citizens’ rights in relation to primary use, including:
- The right to access their electronic health data free of charge
- The right to share health data with healthcare professionals of their choice, including across borders
- The right to download and transmit health data in a structured, commonly used format
- The right to restrict access to specific data elements, subject to clinical and legal safeguards
For healthcare professionals, this translates into improved access to clinically relevant information, especially in cross-border or emergency situations.
The European Electronic Health Record Exchange Format (EEHRxF)
A cornerstone of primary use under the EHDS is the European Electronic Health Record Exchange Format (EEHRxF). The EEHRxF defines the content, structure, and semantic requirements for key categories of health data that must be exchangeable across the EU.
These priority data categories include, among others:
Patient summaries
Electronic prescriptions and dispensations of medication
Laboratory results
Medical imaging reports and images
Hospital discharge reports
The EEHRxF does not replace national EHR systems. Instead, it establishes a common interoperability layer that allows heterogeneous systems to exchange meaningful data. This approach recognises Europe’s diversity while enforcing convergence where it matters most: data semantics, structure, and quality.

Cross-border healthcare and continuity of care
One of the most tangible benefits of primary use under the EHDS is improved cross-border healthcare. Citizens travelling, working, or living in another Member State should no longer face fragmented or inaccessible health information.
Through EHDS-enabled infrastructures, healthcare professionals can access essential patient data—such as allergies, medications, or chronic conditions—provided that the patient consents and legal conditions are met. This reduces medical errors, avoids unnecessary tests, and supports safer clinical decisions.
Importantly, cross-border exchange is not limited to emergencies. The EHDS supports routine care, planned treatments, and long-term follow-up across borders, aligning with the realities of an increasingly mobile European population.
Interoperability as a clinical enabler, not a technical add-on
A key shift introduced by the EHDS is the recognition that interoperability is a clinical requirement, not merely a technical one. Poor interoperability directly affects patient safety, care quality, and professional workload.
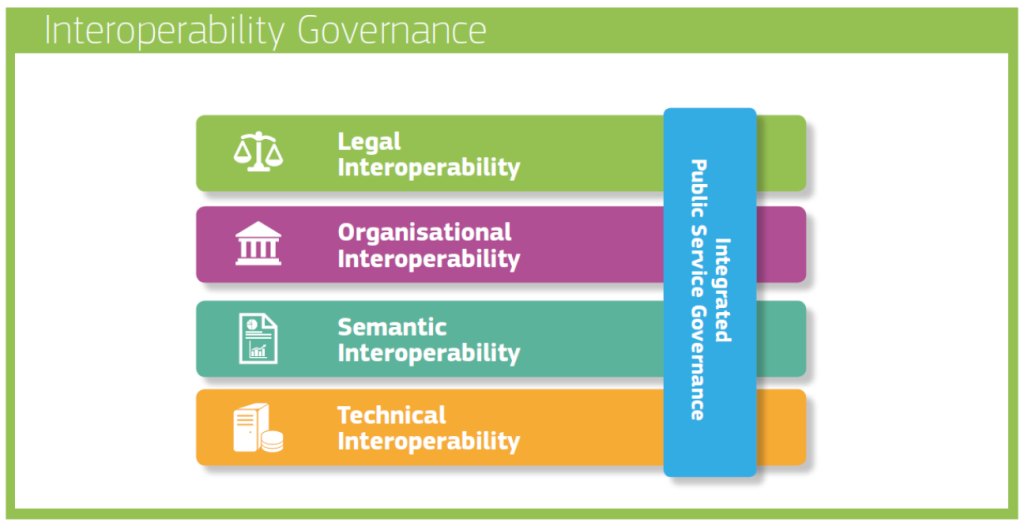
For primary use, interoperability must function at three levels: technical interoperability, enabling systems to exchange data; semantic interoperability, ensuring that the meaning of that data is shared; and organisational interoperability, aligning workflows, roles and governance so interoperability can be applied in real settings.
The European Health Data Space (EHDS) adds a further, essential layer: legal interoperability, by establishing a common legal framework that enables data sharing across organisations and borders in a compliant and trustworthy way. It embeds interoperability obligations into regulation, making compliance mandatory for EHR systems placed on the European market. This has profound implications for healthcare organisations, vendors, and professionals, who must adapt not only systems but also practices.
Workforce readiness and the skills challenge
Implementing primary use under the EHDS is not solely a matter of deploying compliant systems. It requires a workforce capable of using interoperable data effectively and responsibly.
Healthcare professionals, IT developers, system implementers, managers, and policymakers must understand:
- How interoperable health data is structured and exchanged
- What legal and ethical obligations apply to primary use
- How to integrate EHDS-enabled data flows into clinical and operational workflows
- How to ensure data quality, safety, and trust across organisational boundaries
Evidence from European needs analyses highlights persistent gaps in interoperability-related competencies across all professional profiles involved in primary use. Without targeted education and training, the benefits of EHDS-enabled data exchange risk remaining underused or misapplied in practice.
How XiA supports EHDS primary use through capacity building
Addressing this skills gap is central to the mission of Xpanding Innovative Alliance (XiA). XiA supports the implementation of EHDS primary use by focusing on capacity building across the full spectrum of health data stakeholders, from IT developers and system implementers to end users such as clinicians and health managers.
Rather than treating interoperability as a purely technical topic, XiA approaches it as a shared professional competence, embedded in real-world roles and workflows. Its learning approach is structured around modular, practice-oriented building blocks that allow different professional groups to acquire the specific knowledge and skills they need, at the appropriate level of depth.
For IT developers and implementers, this includes competencies related to standards-based data exchange, explaining how EHDS and EEHRxF requirements translate into system design, implementation, and testing. For clinicians and other end users, the focus shifts towards understanding how interoperable data supports clinical decision-making, continuity of care, and patient safety, without requiring them to become technical specialists.
By aligning learning content with practical use cases, regulatory requirements, and professional contexts, XiA contributes to bridging the gap between EHDS policy objectives and day-to-day healthcare practice. In doing so, it supports a workforce that is not only compliant with EHDS obligations, but also capable of realising their clinical and organisational value.
Primary use as the foundation of trust
Trust is central to the EHDS. Citizens will only exercise their rights if they trust that their data is used securely, ethically, and in their interest. Healthcare professionals will only rely on cross-border data if they trust its quality, provenance, and relevance.
Primary use is where this trust is built—or lost. Transparent access rights, clear governance, robust security measures, and professional competence are essential to maintaining confidence in digital health systems. While the EHDS provides the regulatory safeguards, sustained trust ultimately depends on how well professionals are prepared to apply them in practice.
Conclusion
The European Health Data Space marks a turning point for digital health in Europe. While its scope is broad, its success depends fundamentally on the primary use of health data—the everyday use of information to care for patients.
By strengthening patient rights, mandating interoperability through the EEHRxF, and enabling cross-border care, the EHDS creates unprecedented opportunities to improve healthcare quality and safety. At the same time, it places new responsibilities on health systems and professionals.
Primary use under the EHDS is not just a regulatory requirement; it is a transformation of how healthcare is delivered in Europe. Realising this transformation requires not only compliant technology, but also a skilled, confident, and interoperable workforce. Through its focus on targeted, role-aware capacity building, XiA contributes directly to making EHDS primary use operational, meaningful, and sustainable in real clinical settings.
Author : Simon Lewerenz